The Negative Effect of Mouth Breathing on the Body and development of the child.Dr John Flutter
BDS (London) IntroductionI started my first orthodontic case in 1972 when I started in general practice in London. My practice is now limited to orthodontics and dentofacial orthopaedics and I have comprehensive records of all my orthodontic cases for the last twenty five years.
Over the years I have noticed an increasing tendency for children to show evidence of chronic or habitual mouth breathing. This has a negative effect not only on the development of the jaws the shape of the developing cranium and the occlusion but also on the general health of the child.
I have been trying to help children develop nasal breathing for over twenty years. I have discovered more ways that dont work than ways that do! I use several different techniques either separately or together.
There is plenty of evidence in the literature that mouth-breathing has an adverse effect on the growth and development of the face and jaws. All children who are habitual mouth-breathers will have a malocclusion.
The mouth breathers maxillas and mandibles were more retrognathic. Palatal height was higher, overjet was greater in mouth breathers. Overall, mouth breathers had longer faces, with narrower maxillae and retrognathic jaws. (1)
The tongue plays a large part in influencing cranial and maxillary growth. When a child is new born the forward thrusting of the tongue to express milk from the mothers breast is the force that drives the horizontal or forward growth of the maxillae.
The tongue is ideally in contact with the roof of the mouth at rest and during the sub-conscious swallow. In this position, the tongue exerts a lateral force which counterbalances the inward force exerted by the buccinator muscles. This is what maintains the integrity of the eveloping maxilla. When the tongue rests and functions in the palate the teeth erupt around the tongue producing the normal or healthy arch form. The moment the child is a mouth breather, and the tongue drops to the floor of the mouth, the buccinators continue to push inwards and cause the upper arch to collapse.
It is not possible to have the tongue rest and function in the palate and breathe through the mouth. In the chronic mouth breathing child the tongue falls from the roof of the mouth and no longer provides support for the upper arch. This results in a reduced size and retrognathic upper arch.
 |
|
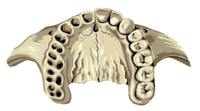
The normal arch form is rounded with the widest part of the maxillae at the mesio-buccal cusps of the upper second molars. This shape is produced when the tongue rests and functions in the palate. In most malocclusions the upper molars are mesially rotated leaving the widest part of the arch at the distal cusps of the upper molars. |
|
When Harvold et al surgically blocked the noses of young monkeys they all developed malocclusions. All experimental animals gradually acquired a facial appearance and dental occlusion different from those of the control animals.
|
|
 |
|
|
|
These are stills from a video of a child displaying a typical mouth breathing pattern. The upper arch is under-developed with a uni-lateral crossbite and an anterior open bite. The posterior cross bite reflects the narrow upper arch unsupported by the tongue and the anterior open bite is a result of the anterior tongue thrust. The upper and lower arches are both retrognathic; the upper arch is more retrognathic leading to the anterior cross bite. |
|
|
|
When assessing a new patient salutary lessons can be learned by looking at the face from a submental view. Chronic mouth breathing has left this young adult with a severely retrognathic maxillae.
When viewed from this direction, the underside of the orbit should not be visible. Two thirds of the floor of the orbit is the maxillae and when the maxillae is retrognathic the eye support is compromised.
The lateral photograph would have been better if I had asked the patient to take her spectacles off before taking the photograph! Even so it is possible to recognise the retrognathic maxillae. |
|